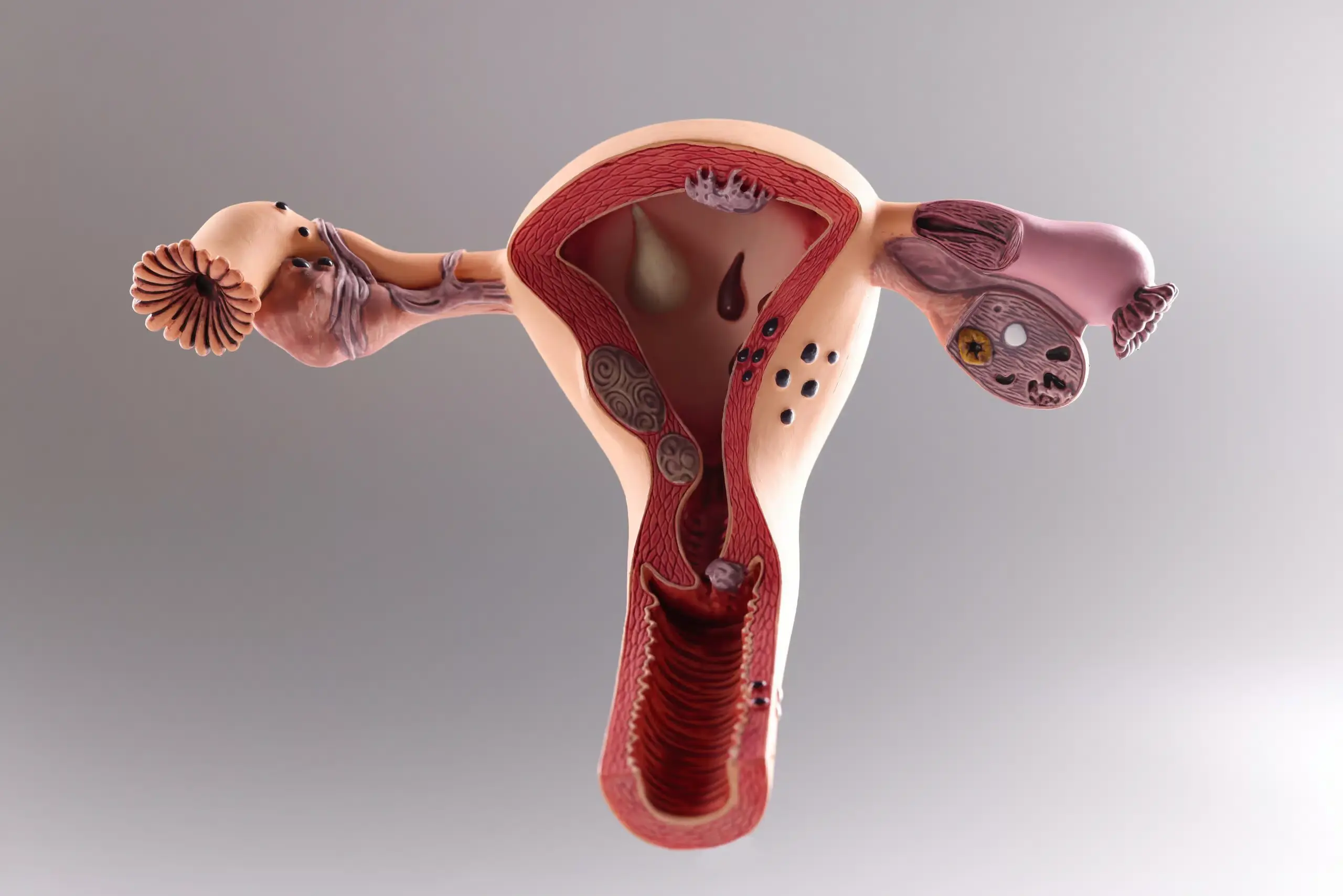
Women often experience changes in menstrual cycles or reproductive health that may seem minor at first but can sometimes indicate underlying gynecological conditions. One such condition is uterine polyps, a relatively common but often overlooked concern affecting women of various age groups. While many uterine polyps remain harmless, some can cause discomfort, irregular bleeding, and fertility complications if left untreated.
Understanding uterine polyps is essential for maintaining reproductive health and recognizing early warning signs. Women frequently ignore abnormal bleeding or menstrual irregularities, assuming they are temporary hormonal fluctuations. However, early evaluation can help prevent complications and improve treatment outcomes.
Specialized gynecological care plays a vital role in diagnosing and managing polyps. With proper medical guidance, women can receive accurate diagnosis, safe treatment, and long term reproductive health support.
Uterine polyps are small growths that develop on the inner lining of the uterus, known as the endometrium. These growths occur when the uterine lining grows excessively and forms tissue projections inside the uterine cavity. Uterine polyps vary in size, ranging from tiny seed like structures to larger growths that may fill a significant portion of the uterus.
Most polyps are non cancerous, but in some cases, they can cause symptoms that affect daily life and reproductive health. Some women may have multiple polyps, while others may develop a single growth. The exact cause is often linked to hormonal imbalance, particularly estrogen fluctuations that stimulate excessive endometrial growth.
Understanding uterine polyps helps women recognize symptoms early and seek timely medical evaluation.
The development of uterine polyps is commonly associated with hormonal changes. Estrogen plays a key role in regulating the growth of the uterine lining. When estrogen levels remain elevated or unbalanced, the endometrial tissue may grow excessively, leading to the formation of uterine polyps.
Certain health conditions increase the likelihood of developing polyps. Women experiencing obesity, high blood pressure, or hormonal disorders may have a higher risk. Age is another contributing factor, as uterine polyps are more frequently diagnosed in women approaching menopause, although they can occur at any reproductive stage.
Lifestyle factors such as chronic stress, poor metabolic health, and irregular hormonal cycles may also contribute to the formation of uterine polyps. Identifying these risk factors helps guide treatment and prevention strategies.
Many women with uterine polyps may not experience noticeable symptoms. However, when symptoms occur, they usually involve changes in menstrual patterns or abnormal bleeding.
One of the most common signs of polyps is irregular menstrual cycles. Women may notice unpredictable bleeding between periods or unusually frequent cycles. Heavy menstrual bleeding is another frequent symptom, often leading to fatigue and reduced daily comfort.
Some women experience spotting after menopause, which should always be evaluated by a gynecologist. In certain cases, uterine polyps may cause difficulty in conceiving or maintaining pregnancy. Pelvic discomfort or pressure may occur when polyps grow larger.
Recognizing these symptoms early allows timely diagnosis and effective treatment.
Uterine polyps can interfere with fertility by altering the environment of the uterus. These growths may block sperm movement, prevent embryo implantation, or disrupt the uterine lining required for pregnancy support.

Women struggling with unexplained infertility are often evaluated for uterine polyps as part of fertility assessment. Removing polyps can improve uterine health and increase the chances of successful conception.
Early diagnosis is especially important for women planning pregnancy, as untreated polyps may affect reproductive outcomes.
Several factors increase the likelihood of developing uterine polyps. Women experiencing hormonal imbalance, irregular ovulation, or metabolic disorders may be at higher risk. Age related hormonal changes during perimenopause also contribute to polyp formation.
Certain medications that influence estrogen levels may increase risk. Women with a history of uterine conditions or reproductive disorders may also be more susceptible.
Understanding risk factors helps healthcare providers recommend preventive strategies and early screening when necessary.
Accurate diagnosis of uterine polyps requires medical evaluation and imaging techniques. Gynecologists often begin with a detailed review of menstrual history and symptoms. Pelvic ultrasound is commonly used to visualize the uterine lining and detect abnormal growths.
In some cases, specialized diagnostic procedures may be recommended to examine the uterine cavity more closely. These procedures allow gynecologists to confirm the presence, size, and location of uterine polyps.
Timely diagnosis helps determine whether treatment is required and prevents complications related to untreated polyps.
Treatment for uterine polyps depends on symptoms, size of the polyp, reproductive goals, and overall health condition. Small uterine polyps without symptoms may only require monitoring and regular follow up examinations.
Medical treatment may be recommended to regulate hormonal imbalance and reduce polyp growth. Hormonal therapies help control excessive endometrial tissue growth and improve menstrual regularity.
Surgical removal is often recommended when polyps cause heavy bleeding, fertility problems, or persistent symptoms. Minimally invasive procedures allow safe removal of polyps while preserving uterine health.
Early treatment improves reproductive outcomes and reduces the risk of recurrence or complications.
Most polyps are benign and do not pose serious health threats. However, a small percentage may develop abnormal or precancerous changes, especially in postmenopausal women. Regular gynecological evaluation helps detect these changes early.
Women experiencing postmenopausal bleeding should always undergo medical assessment to rule out serious conditions. Early diagnosis ensures appropriate treatment and reduces health risks.
Although uterine polyps cannot always be prevented, maintaining hormonal balance and reproductive health reduces risk. Healthy lifestyle habits such as balanced nutrition, regular physical activity, and stress management support hormonal stability.
Routine gynecological checkups help detect uterine polyps at an early stage. Monitoring menstrual patterns and seeking medical advice for abnormal bleeding also plays a significant role in prevention.
Preventive care supports long term reproductive health and early detection of gynecological conditions.
Women should consider medical consultation if they experience irregular menstrual bleeding, unusually heavy periods, postmenopausal spotting, or difficulty conceiving. These symptoms may indicate uterine polyps or other reproductive health concerns.
Seeking early medical evaluation ensures accurate diagnosis and effective treatment. Ignoring abnormal bleeding may lead to complications or delayed management.
Dr. Namrata Jadhav specializes in diagnosing and managing polyps using advanced gynecological techniques and patient centered care. She focuses on identifying underlying hormonal and reproductive factors contributing to polyp formation.
Her approach emphasizes thorough evaluation, personalized treatment planning, and minimally invasive procedures when necessary. She prioritizes patient education, helping women understand their condition and treatment options in a comfortable and supportive environment.
Through her expertise, patients receive comprehensive reproductive health care that addresses both symptoms and long term wellness goals.
Most women experience significant symptom relief after treatment for uterine polyps. Surgical removal often improves menstrual regularity and fertility outcomes. Regular follow up examinations help monitor uterine health and detect recurrence early.
Women planning pregnancy often benefit from timely treatment, as improved uterine environment supports successful conception and pregnancy maintenance.
Maintaining hormonal balance and attending routine gynecological checkups supports long term reproductive health after treatment.
Uterine polyps are a common gynecological condition that can affect menstrual health, fertility, and overall reproductive wellness. While many polyps remain harmless, symptoms such as irregular bleeding, heavy periods, and fertility challenges should never be ignored.
Early diagnosis and personalized treatment help prevent complications and improve reproductive outcomes. With expert evaluation, advanced diagnostic techniques, and patient focused care, women can effectively manage uterine polyps and maintain healthy reproductive function.
Prioritizing routine gynecological checkups and seeking timely medical advice ensures long term reproductive health and peace of mind.
Women Health By Dr. Namrata Jadhav 2025 | All Rights Reserved.
Need help? Chat with us