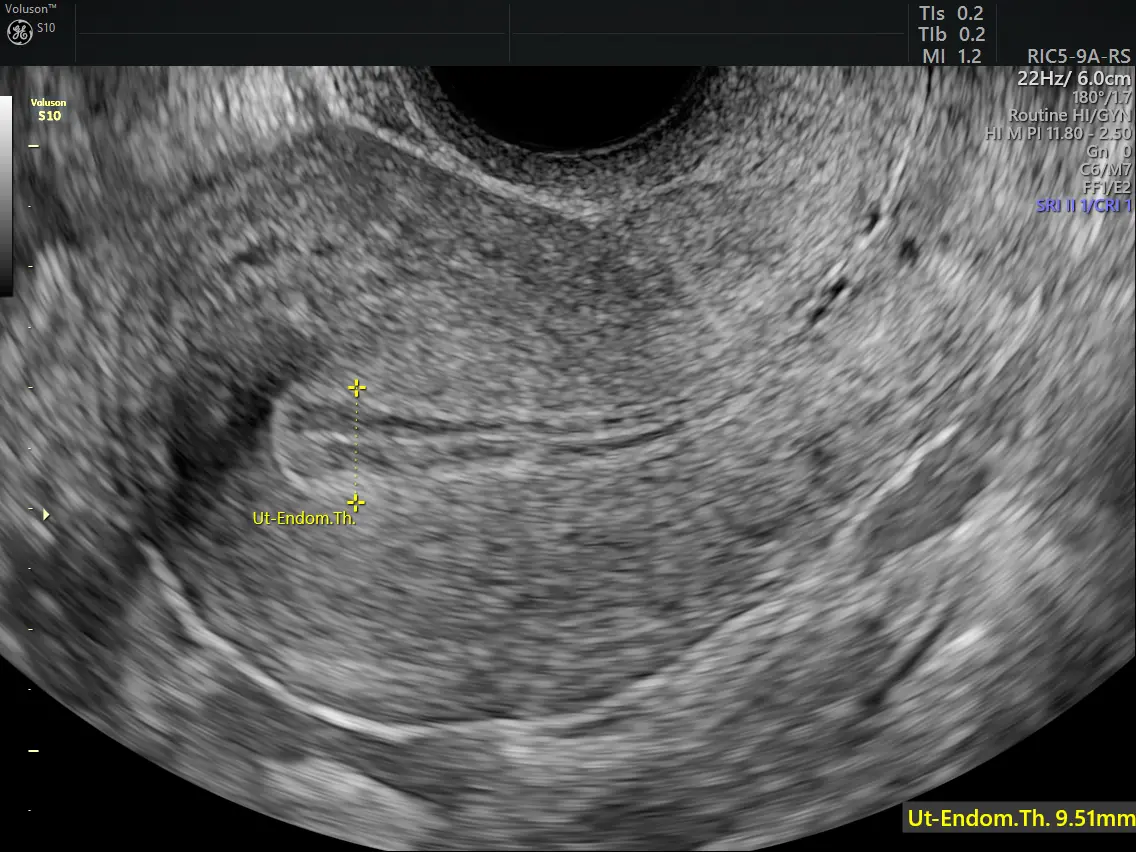
Changes in menstrual patterns are often the first sign that something within the reproductive system may need attention. While many irregularities are linked to temporary hormonal fluctuations, some may indicate underlying conditions that require medical evaluation. One such condition is endometrial hyperplasia, a disorder involving abnormal thickening of the uterine lining.
Endometrial hyperplasia develops when the endometrium, the inner lining of the uterus, grows excessively due to hormonal imbalance—most commonly excess estrogen without adequate progesterone. While the condition is treatable, delayed diagnosis may increase the risk of complications, including progression to endometrial cancer in certain cases.
Understanding endometrial hyperplasia is essential for protecting long-term reproductive and hormonal health. With early evaluation, proper diagnosis, and personalized treatment, women can effectively manage this condition and maintain uterine health.
Endometrial hyperplasia refers to the abnormal thickening of the uterine lining caused by excessive stimulation from estrogen. During a normal menstrual cycle, estrogen stimulates the growth of the endometrium, and progesterone stabilizes it. If pregnancy does not occur, hormone levels drop and menstruation begins.
However, when ovulation does not occur regularly, progesterone may not be produced in sufficient amounts. This results in continuous estrogen stimulation without balance, causing the endometrium to thicken excessively. Over time, this abnormal thickening may lead to irregular bleeding and other symptoms.
Endometrial hyperplasia can occur in women of reproductive age but is more common during perimenopause and postmenopause, when hormonal fluctuations are more frequent.
Endometrial hyperplasia is classified based on whether abnormal cells are present in the uterine lining. This classification helps determine the risk level and appropriate treatment approach.
This type involves thickening of the uterine lining without significant cellular abnormalities. It carries a lower risk of progressing to cancer and is often manageable with hormonal treatment.
In this type, the glandular structure of the endometrium becomes more crowded and irregular. While still manageable, it requires careful monitoring and treatment.
Atypical hyperplasia involves abnormal cell changes and carries a higher risk of progressing to endometrial cancer if left untreated. Prompt diagnosis and targeted treatment are essential in such cases.
Proper classification through biopsy and pathological evaluation plays a critical role in guiding management decisions.
The primary cause of endometrial hyperplasia is prolonged exposure to estrogen without adequate progesterone. This imbalance can occur due to several underlying factors.
Women with irregular ovulation patterns, such as those with polycystic ovary syndrome, are at higher risk. Obesity also contributes, as excess fat tissue can increase estrogen production. Perimenopausal women frequently experience hormonal fluctuations that may lead to anovulatory cycles and unopposed estrogen exposure.
Hormone replacement therapy containing estrogen without progesterone may increase risk in postmenopausal women. Certain medical conditions affecting ovarian function can also contribute to hormonal imbalance.
Identifying the underlying cause is essential for effective treatment and prevention of recurrence.
Abnormal uterine bleeding is the most common symptom of endometrial hyperplasia. Women may experience heavy menstrual bleeding, prolonged periods, or bleeding between cycles.
In perimenopausal women, cycles may become unpredictable and heavier than usual. Postmenopausal bleeding is particularly concerning and should always be evaluated promptly.
Some women may not notice symptoms initially, which is why routine gynecological checkups are important. Early detection allows timely management and reduces potential complications.
Several risk factors increase the likelihood of developing endometrial hyperplasia. Age is a significant factor, especially during perimenopause and postmenopause. Obesity increases estrogen production and contributes to hormonal imbalance.
Women with chronic anovulation, such as those with PCOS, face higher risk. A history of infertility, diabetes, or high blood pressure may also contribute. Family history of endometrial or colorectal cancer may increase overall risk.
Understanding these risk factors helps guide screening and preventive strategies.
Endometrial hyperplasia can disrupt normal uterine function and interfere with implantation. Women experiencing irregular ovulation due to hormonal imbalance may find it difficult to conceive.
In cases where hyperplasia is treated early, fertility outcomes can improve significantly. Hormonal regulation often restores normal ovulatory cycles and supports healthy uterine lining development.
Women planning pregnancy should seek early evaluation if experiencing persistent menstrual irregularities.
Diagnosis begins with a detailed medical history and evaluation of menstrual patterns. Pelvic ultrasound is commonly used to measure endometrial thickness and detect abnormalities.
If abnormal thickening is suspected, an endometrial biopsy is performed to examine the tissue under a microscope. This step is crucial in identifying whether atypical cells are present and determining the appropriate treatment plan.
Accurate diagnosis ensures safe and effective management while reducing unnecessary interventions.
Treatment depends on the type of hyperplasia, age, reproductive goals, and overall health condition.
Progesterone therapy is commonly used to counteract excess estrogen and regulate the uterine lining. It may be administered orally, through injections, or via intrauterine systems.
Hormonal therapy often successfully reverses simple and some complex cases of endometrial hyperplasia.
In cases of atypical hyperplasia or when hormonal therapy is ineffective, surgical intervention may be recommended. Procedures may include targeted removal of abnormal tissue.
In severe or high risk cases, especially in postmenopausal women who have completed childbearing, more definitive treatment may be considered after thorough medical evaluation.
Treatment decisions are always personalized based on individual needs and risk factors.
While many cases of endometrial hyperplasia remain benign, atypical forms carry an increased risk of progressing to endometrial cancer. Early detection significantly reduces this risk.
Regular follow up and appropriate treatment help prevent progression. Women experiencing postmenopausal bleeding should seek immediate medical attention, as early intervention is key to favorable outcomes.
Maintaining hormonal balance is essential in preventing endometrial hyperplasia. Healthy weight management reduces excess estrogen production. Regular physical activity supports metabolic and hormonal health.
Managing conditions such as PCOS and diabetes lowers risk. Women undergoing hormone replacement therapy should ensure balanced estrogen and progesterone regimens under medical supervision.
Routine gynecological examinations play a vital role in early detection and prevention.
Women should seek medical advice if they experience heavy menstrual bleeding, bleeding between periods, or postmenopausal spotting. Persistent irregular cycles also warrant evaluation.
Early consultation allows accurate diagnosis and prevents complications. Ignoring symptoms may delay treatment and increase risk.
Dr. Namrata Jadhav specializes in diagnosing and managing endometrial hyperplasia through comprehensive evaluation and evidence based treatment strategies. Her approach focuses on identifying underlying hormonal imbalances and tailoring treatment to individual reproductive goals.
She emphasizes early detection, accurate classification, and personalized management plans to ensure optimal uterine health. By combining advanced diagnostic techniques with compassionate care, she supports women in maintaining long term reproductive wellness.
Her patient centered approach ensures that women understand their diagnosis, treatment options, and follow up care requirements with clarity and confidence.
With timely diagnosis and appropriate treatment, most women recover successfully from endometrial hyperplasia. Regular monitoring helps prevent recurrence and ensures early detection of any changes.
Women who maintain healthy lifestyle habits and attend routine gynecological checkups significantly reduce long term risks. Proper hormonal balance remains central to ongoing uterine health.
Endometrial hyperplasia is a treatable condition characterized by abnormal thickening of the uterine lining due to hormonal imbalance. While often manageable, early diagnosis is essential to prevent complications and reduce cancer risk.
Recognizing symptoms such as abnormal bleeding and seeking timely medical care ensures effective treatment and long term reproductive health. Through expert evaluation, personalized management, and preventive care, women can successfully maintain healthy uterine function and hormonal balance.
Women Health By Dr. Namrata Jadhav 2025 | All Rights Reserved.
Need help? Chat with us