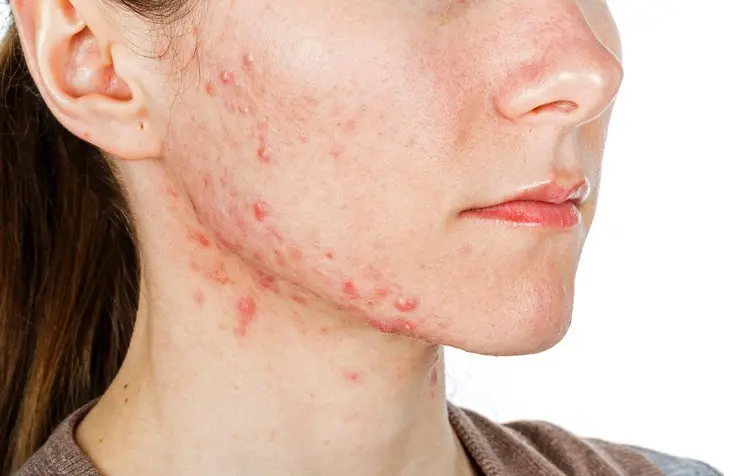
Acne is often associated with teenage years, but many women continue to experience breakouts well into adulthood. When acne appears due to fluctuations in hormones rather than typical skin-related factors, it is commonly referred to as hormonal acne.
Hormonal acne in women can be frustrating because it tends to recur regularly and may not respond well to standard skincare treatments. Breakouts often appear during certain phases of the menstrual cycle, pregnancy, or other hormonal changes, making them more difficult to control without addressing the underlying cause.
While hormonal acne is primarily visible on the skin, it is usually linked to internal hormonal imbalances that affect oil production and inflammation. Understanding the root causes, identifying symptoms, and seeking appropriate medical care are essential steps toward managing this condition effectively.
With proper evaluation and targeted treatment, women can significantly reduce breakouts, improve skin health, and restore hormonal balance.
Hormonal acne refers to acne breakouts triggered by fluctuations in hormone levels, particularly androgens. These hormones stimulate the sebaceous glands in the skin, causing them to produce excess oil (sebum).
When excess oil combines with dead skin cells and bacteria, pores become clogged, resulting in acne lesions such as blackheads, whiteheads, and inflamed pimples.
Unlike typical acne that may affect teenagers, hormonal acne is more common in adult women and often appears along the lower face, jawline, chin, and neck.
The condition may develop gradually or appear suddenly during times of hormonal change. Because the root cause lies in hormonal regulation, addressing internal factors is often necessary for long-term improvement.
Hormones play a major role in regulating skin health. Estrogen, progesterone, and androgens influence oil production, skin cell turnover, and inflammation levels.
Androgens, which are present in both men and women, stimulate the sebaceous glands. When androgen levels rise or become dominant relative to other hormones, oil production increases.
Excess oil can clog hair follicles and create an environment where acne-causing bacteria thrive. The resulting inflammation leads to painful breakouts that can persist or recur.
Hormonal fluctuations may occur during menstrual cycles, pregnancy, menopause, or certain medical conditions, all of which can contribute to hormonal acne.
Several factors can trigger hormonal acne in women. Identifying the underlying cause helps guide appropriate treatment.
Hormone levels change naturally throughout the menstrual cycle. Many women experience breakouts a few days before their period due to shifts in estrogen and progesterone levels.
PCOS is a hormonal disorder that can increase androgen levels in the body. This imbalance often leads to persistent acne, irregular periods, and other symptoms.
Chronic stress increases cortisol production, which can indirectly affect androgen levels and worsen acne breakouts.
Hormonal changes during pregnancy and after childbirth may influence skin oil production, sometimes causing acne flare-ups.
Some contraceptive methods may influence hormone levels and trigger acne in certain individuals.
As women approach menopause, hormonal fluctuations can lead to adult-onset acne or worsening of existing skin conditions.
Understanding these triggers is essential for choosing the most effective treatment strategy.
Hormonal acne often presents differently from typical acne. The breakouts tend to follow predictable patterns linked to hormonal fluctuations.
Common symptoms include:
Because these symptoms may indicate underlying hormonal imbalance, medical evaluation may be necessary when acne becomes persistent or severe.
Skin conditions often impact more than physical appearance. Persistent acne can affect self-confidence, emotional wellbeing, and social interactions.

Women dealing with recurring hormonal acne may feel frustrated when common skincare treatments fail to produce lasting results. Anxiety, embarrassment, and lowered self-esteem are common emotional effects.
Addressing hormonal acne with a comprehensive medical approach not only improves skin health but also supports psychological wellbeing.
Diagnosing hormonal acne involves more than examining the skin. Healthcare providers often evaluate hormonal patterns and reproductive health to determine the underlying cause.
Evaluation may include:
Medical history review
Menstrual patterns, lifestyle habits, and medication use can provide valuable clues.
Hormonal blood tests
Hormone levels such as estrogen, progesterone, testosterone, and thyroid hormones may be assessed.
Pelvic ultrasound
If PCOS is suspected, imaging may help evaluate ovarian health.
Skin examination
Dermatological assessment helps determine acne severity and type.
This comprehensive approach ensures that treatment addresses both skin symptoms and underlying hormonal factors.
Treatment for hormonal acne focuses on regulating hormone levels and reducing skin inflammation.
Certain medications help balance hormones and reduce androgen effects on the skin.
In some women, combined hormonal contraceptives help stabilize estrogen and progesterone levels, improving acne symptoms.
Medications that block androgen activity may reduce excess oil production and prevent new breakouts.
Dermatological treatments such as retinoids or antibacterial creams may be used alongside hormonal therapy.
Diet, stress management, and proper skincare routines can complement medical therapy.
Treatment plans are always personalized depending on the underlying hormonal cause and the patient’s health profile.
In addition to medical care, certain lifestyle changes can support skin and hormonal health.
Helpful strategies include:
These habits support hormonal balance and may help reduce acne severity over time.
While occasional breakouts are normal, persistent or severe acne should not be ignored.
Women should consider consulting a specialist if they experience:
Early evaluation helps identify hormonal issues and prevent long-term skin scarring.
Women experiencing persistent hormonal acne may benefit from a comprehensive gynecological and hormonal evaluation. Dr. Namrata Jadhav provides expert assessment of hormonal health and reproductive conditions that may contribute to acne and other symptoms.
Her approach focuses on identifying the underlying hormonal imbalance rather than treating skin symptoms alone. Through personalized treatment strategies and evidence-based medical care, she helps patients address both hormonal health and skin concerns.
By combining gynecological expertise with a patient-centered approach, she supports women in achieving long-term hormonal balance and improved overall wellbeing.
Although hormonal fluctuations cannot always be prevented, certain preventive strategies can help reduce the frequency and severity of breakouts.
Maintaining hormonal balance through healthy lifestyle habits, routine medical checkups, and proper skincare can significantly improve skin health. Monitoring menstrual cycles and recognizing early hormonal symptoms also helps women seek timely medical care.
Consistent self-care and professional guidance are key to managing hormonal acne effectively.
Hormonal acne is a common yet often misunderstood condition affecting many women beyond adolescence. Driven by fluctuations in hormone levels, these breakouts can be persistent and emotionally challenging.
Understanding the causes of hormonal acne, recognizing its symptoms, and seeking proper medical evaluation are essential steps toward effective treatment. With the right combination of medical care, lifestyle adjustments, and supportive skincare practices, most women can achieve healthier skin and improved hormonal balance.
Addressing the root hormonal cause not only helps control acne but also contributes to better reproductive and overall health.
Women Health By Dr. Namrata Jadhav 2025 | All Rights Reserved.
Need help? Chat with us